
Breaking News
 Tina Peters, granted clemency by Colorado's Dem governor
Tina Peters, granted clemency by Colorado's Dem governor
 Tulsi Gabbard at center of explosive CIA claim as JFK and MKUltra files 'vanish from her office*
Tulsi Gabbard at center of explosive CIA claim as JFK and MKUltra files 'vanish from her office*
 Bessent Says US, China To Launch AI Safety Talks After Trump-Xi Meeting In Beijing
Bessent Says US, China To Launch AI Safety Talks After Trump-Xi Meeting In Beijing
 Cuba Depletes Fuel As Blackouts Worsen, Putting Havana's Communists Under Pressure...
Cuba Depletes Fuel As Blackouts Worsen, Putting Havana's Communists Under Pressure...
Top Tech News
 US To Develop Small Modular Nuclear Reactors For Commercial Shipping
US To Develop Small Modular Nuclear Reactors For Commercial Shipping
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
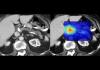 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
A multi-terrain robot from China is going viral, not because of raw speed or power...
 The World's Biggest Fusion Reactor Just Hit A Milestone
The World's Biggest Fusion Reactor Just Hit A Milestone
 Wow. Researchers just built an AI that can control your body...
Wow. Researchers just built an AI that can control your body...
 Google Chrome silently installs a 4 GB AI model on your device without consent
Google Chrome silently installs a 4 GB AI model on your device without consent
 The $5 Battery That Never Dies - Edison Buried This 100 Years Ago
The $5 Battery That Never Dies - Edison Buried This 100 Years Ago
MIT's "living drug factories" produce insulin from inside the body
For the last couple of decades, a relatively small amount of diabetics have benefited from what's known as pancreatic islet cell transplantation. These are the cells that produce insulin in a functional pancreas and by implanting them into sufferers of diabetes, they can take on their traditional role and negate the need for regular insulin injections.
The reason this form of therapy isn't used more widely is that the great majority of recipients experience complications, as their immune system mistakes the transplanted cells for dangerous invaders and goes on the attack. Drugs that suppress this immune response are one solution, but they invite their own risks such as vulnerability to infection or more serious side effects.
So getting pancreatic islet cells to survive transplantation and function as normal is seen as a key objective by researchers in the field. Converting the patient's own liver cells into islet cells, wrapping them in seaweed-based capsules and organizing them into clusters are just a few of the ways the process may be improved, and now scientists at MIT have come up with another.
The technology involves encapsulating the cells in a protective shell made from a silicon-based elastomer, combined with a porous membrane. These pores are large enough that nutrients, oxygen and insulin can move freely through the membrane, but small enough to keep out immune cells that seek to attack the cell.



