
Breaking News
 India Stock Market Loses 5.5 Trillion Rupees Amid Energy Crisis
India Stock Market Loses 5.5 Trillion Rupees Amid Energy Crisis
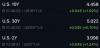 US Bond Market Crisis Intensifies Amid Rising Yields
US Bond Market Crisis Intensifies Amid Rising Yields
 Critical Minerals Supply Chain Under Siege Amid Geopolitical Tensions
Critical Minerals Supply Chain Under Siege Amid Geopolitical Tensions
 BEANS, BEEF AND BOEING: PPI INFLATION TAKES FLIGHT
BEANS, BEEF AND BOEING: PPI INFLATION TAKES FLIGHT
Top Tech News
 US To Develop Small Modular Nuclear Reactors For Commercial Shipping
US To Develop Small Modular Nuclear Reactors For Commercial Shipping
 New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
New York Mandates Kill Switch and Surveillance Software in Your 3D Printer ...
 Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
Cameco Sees As Many As 20 AP1000 Nuclear Reactors On The Horizon
 His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
His grandparents had heart disease.
At 11, Laurent Simons decided he wanted to fight aging.
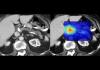 Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
Mayo Clinic's AI Can Detect Pancreatic Cancer up to 3 Years Before Diagnosis–When Treatment...
A multi-terrain robot from China is going viral, not because of raw speed or power...
 The World's Biggest Fusion Reactor Just Hit A Milestone
The World's Biggest Fusion Reactor Just Hit A Milestone
 Wow. Researchers just built an AI that can control your body...
Wow. Researchers just built an AI that can control your body...
 Google Chrome silently installs a 4 GB AI model on your device without consent
Google Chrome silently installs a 4 GB AI model on your device without consent
 The $5 Battery That Never Dies - Edison Buried This 100 Years Ago
The $5 Battery That Never Dies - Edison Buried This 100 Years Ago
First-ever drug to repair DNA and regenerate damaged tissue is here
Researchers at Cedars-Sinai made the breakthrough after first developing a technique to isolate progenitor cells from the heart. These cells, much like stem cells, can form new healthy tissue but in a more targeted way. In other words, these cells taken from the heart can help restore function to that organ.
Medical scientist Eduardo Marbán – then at Johns Hopkins and now Cedars-Sinai – found that heart progenitor cells also have a special mechanism where they send out sacs, known as exosomes, which carry molecules of DNA, RNA and protein between cells and can repair and regenerate damaged tissue.
"Exosomes are like envelopes with important information," said first author Ahmed Ibrahim, PhD, MPH, an associate professor in the Department of Cardiology in the Smidt Heart Institute. "We wanted to take apart these coded messages and figure out which molecules were, themselves, therapeutic."
The team worked to unpack what was in those healing sacs, sequencing the exosomal RNA material and finally landeing on one molecule that was more prominent than others. Focusing on this one RNA molecule, animal studies confirmed the researchers' hypothesis that it played a key role in facilitating tissue repair.
Fast-forward two decades and the scientists have finally fabricated this naturally occurring RNA molecule in the lab – the synthetic healer known as TY1.
"By probing the mechanisms of stem cell therapy, we discovered a way to heal the body without using stem cells," said senior author Marbán, MD, PhD, executive director of the Smidt Heart Institute at Cedars-Sinai. "TY1 is the first exomer – a new class of drugs that address tissue damage in unexpected ways."
TY1 has the structure of existing RNA drugs, and works like its natural version – amplifying the activity of the Trex1 gene, which increases the activity of immune cells that rally around damaged DNA and clear out the junk, allowing for the repair and regeneration to take place. This process is critical in the wake of a heart attack to minimize cellular scarring left from the event.
Studies have demonstrated that DNA damage plays a critical role in the development of pressure overload–induced heart failure, dilated cardiomyopathy and aging-related cardiac conditions, and this damage to myocardial tissue is a large factor in how well someone recovers from a heart attack. Essentially, the less damage you have the better your long-term prognosis. Stimulating the cellular "recovery team," through this novel experimental drug, boosts the body's ability to repair itself.
And it doesn't stop at heart tissue damage repair.
"By enhancing DNA repair, we can heal tissue damage that occurs during a heart attack," Ibrahim said. "We are particularly excited because TY1 also works in other conditions, including autoimmune diseases that cause the body to mistakenly attack healthy tissue. This is an entirely new mechanism for tissue healing, opening up new options for a variety of disorders."
Following on from animal models, TY1 will next be studied in a clinical trial. If the drug performs as expected in humans, it paves the way for a new class of therapeutics that can help mitigate a broad range of cellular damage caused by both sudden adverse events and chronic inflammatory conditions.



